II. History
- Word "Croup" derived from Scottish for raven's "croak"
III. Epidemiology
-
Incidence
- Overall Incidence: 3-6 cases per 100 children <6 years
- Accounts for 15% of pediatric respiratory visits to the emergency department
- Hospitalizations: 1-8% of US cases (20,000 per year)
- Intubation: 1-5% of cases hospitalized
- Boys affected more than girls by ratio of 1.5 to 1
- Outbreaks and epidemics occur in autumn to early winter
- Can occur year round sporadically
- Affects ages under 6 years (rarely up to 8 to 12 years)
- Most common cause of Stridor in children 6 months to 3 years of age
- Typical age 6 months to 36 months of age (peaks between 12 and 24 months)
- Rare before 3 months of age
IV. Pathophysiology
- Subglottic infection, inflammation and edema
- Tracheal edema at the most narrow aspect of a child's airway
- Subglottic area is 4 mm in a typical infant (and croup may decrease this to 2 mm area)
- Every mm of airway area lost results in a loss of air flow volume to the power of 4 (Poiseuille's law)
V. Causes
- Parainfluenza virus (50-75% of cases)
- Type 1 (most common type, 18% of cases)
- Type 2
- Type 3 (more common in younger children)
- Adenovirus
- Respiratory Syncytial Virus (RSV)
- Influenza A and Influenza B
- Rhinovirus
- Enteroviruses
- Human Bocavirus (spring and fall)
- Mycoplasma pneumoniae (uncommon)
- Corynebactgerium Diphtheriae (uncommon)
VI. Symptoms
- Low grade fever (or affebrile in some cases)
- High grade fever suggests other diagnosis (see differential diagnosis)
- Prodrome of initially mild upper respiratory symptoms or Coryza (first 1-2 days)
- Nasal Congestion
- Rhinorrhea
- Upper respiratory symptoms rapidly develop with abrupt onset
- Hoarseness
- Cough: "Barking" OR "seal-like"
- Inspiratory Stridor
- Expiratory Wheezing
- Dyspnea
- Symptoms worse at night
- Symptom duration <1 week (peaks at 2-4 days)
- Cough may persist up to 1 week
VII. Signs
- "Sound worse than they look" (Opposite of Epiglottitis)
- However, severe croup can cause complete airway obstruction
- Minimal Wheezing (Inspiratory Stridor instead)
- Minimal rhonchi and no rales
- Moderate respiratory distress
- Nasal flaring
- Respiratory retractions
- Inspiratory Stridor
VIII. Labs
- Avoid labs unless diagnosis unclear
- Blood draws cause worsening distress and do not add to diagnosis in typical croup
-
Complete Blood Count
- May show mild Leukocytosis
- May distinguish from the high white counts in Bacterial causes in differential diagnosis
IX. Diagnosis
- See Croup Score
- Croup accounts for 99% of abrupt onset of Stridor
- However, consider the atypical case in the differential diagnosis as below
X. Course
- Mild Cases: 85%
- Hospitalized: 5%
- Severe Cases: 1%
- Intubated: 0.05% of croup cases
- Mortality <0.5% (even for intubated patients)
XI. Differential Diagnosis (Croup is diagnosis of exclusion)
- See Pediatric Airway Obstruction Causes
- Angioedema
-
Epiglottitis (3-12 years old)
- Less common in U.S. now since HaemophilusInfluenzae type B Immunization
- High fever, Drooling, muffled voice, Pharyngitis
- Cough (esp. barking cough) is more likely to be croup
-
Bacterial Tracheitis (<6 years old)
- High fever with signs of toxicity and rapid decompensation
- Ludwig's Angina
- Peritonsillar Abscess
- Retropharyngeal Abscess
- Diphtheria
- Paraquat Poisoning (Herbicides)
- Smoke Inhalation
-
Foreign Body Aspiration (esp. < 3 years old)
- History of Choking episode (88%)
- Neck XRay PA and Lateral if object is radiopaque
-
Gastroesophageal Reflux
- Common cause of recurrent croup
- Airway lesion (Hemangioma, laryngeal mass)
XII. Imaging
- Avoid imaging (as with labs) unless diagnosis is unclear
- Typically worsens distress and does not add to diagnosis in typical croup
- Avoid CT neck in children (radiation risk) unless high suspicion for lesion
- Lateral Neck XRay
- Findings suggestive of croup
- "Steeple" sign on PA Neck XRay (40-50% of croup cases)
- Narrowing of subglottic region from mucosal edema
- Dilated hypopharynx (most sensitive finding)
- Images
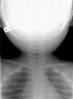 From MedPix with permission.
From MedPix with permission.
- Findings suggestive of alternative diagnosis
- Epiglottitis: Thickened epiglottis
- Retropharyngeal Abscess: Widening retropharyngeal soft tissue
- Bacterial Tracheitis: Thickened trachea
- Findings suggestive of croup
-
Chest XRay
- Does not diagnose croup (will not demonstrate steeple sign)
- Indicated only to evaluate differential diagnosis (e.g. Pneumonia) where the diagnosis is unclear
- Other diagnostics
- Laryngoscopy
- May be considered (only with caution) in suspected Epiglottitis
- Laryngoscopy
XIII. Management: Home Therapy
- Maintain adequate Ambient humidity in house
- Cool mist may decrease subglottic edema
- No studies to support this
- May make Asthma worse due to irritation
- Theoretically decreases tracheal mucosal edema and secretion viscosity
- Options
- Cool-mist humidifier
- Cold Weather
- Bundle child warmly
- Bring outside for 15 minutes
- Closed bathroom with cold shower mist
- Maintain adequate hydration
- Offer child favorite drink every 10 minutes
- Consider crushed ice drinks or other frozen treats
- Corticosteroids
XIV. Management: Emergency Department and Inpatient
- See Severe Croup management and delayed sequence protocol described below
- Primary tenet
- Do not distress a child with croup
- Avoid unnecessary procedures (e.g. delay Intravenous Access until stable)
- Position child as they are most comfortable
- Oxygen
- Indicated for Hypoxia or moderate to severe respiratory distress
- Humidified oxygen offers no benefit over non-humidified oxygen in moderate croup
- Blow-by oxygen is preferred to avoid distressing child
- Do not use heated humidification due to risk of burns
-
Corticosteroids
- See Dexamethasone in Croup (includes Nebulized Budesonide in Croup)
- Indicated in all croup cases, regardless of severity
- Single dose lasts 60-72 hours and should cover the entire croup episode (typically 2-5 days)
- Most important single treatment in croup
- Has decreased croup mortality 200% from before 1990 to now (from 0.5% to 0.03%)
- Dexamethasone
- Typical dose (esp. severe cases): 0.6 mg/kg orally (maximum 10-16 mg)
- Dose of 0.15 to 0.3 mg/kg as effective as 0.6 mg/kg in mild to moderate cases
- Onset of action in 6 hours and effect lasts for 72 hours
- Oral is preferred over Parenteral dosing (give 1 mg/ml concentrated IV solution orally)
- Dexamethasone is preferred over Budesonide
-
Nebulized racemic epinephrine
- Indicated in moderate to severe emergency department cases with signs of respiratory distress
- Alpha-Agonist effect Vasoconstricts, decreasing mucosal edema
- Beta agonsit effect increases Smooth Muscle relaxation as well as thinning tracheal secretions
- Nebulizer Dose
- Racemic Epinephrine 0.05 ml/kg (maximum 0.5 ml) of 2.25% in 2 ml saline via nebulizer or
- Standard L-Epinephrine 0.5 ml/kg (maximum 5 ml) of 1:1,000 in 2 ml saline via nebulizer
- As effective as Racemic Epinephrine and widely available in all ERs without special ordering
- Effect onset within 30 minutes and lasts up to 2 hours (some effects may persist up to 4 hours)
- Observe at least 2 hours after administration (some recommend 3 hours)
- If no recurrent Stridor, may discharge home after 2-3 hours
- Most croup decompensations will occur 1 to 1.5 hours after nebulized Epinephrine
- If Stridor recurs may give one additional Epinephrine neb and observe for additional 2-3 hours
- Dexamethasone may be taking effect by this time (~6 hours from dose)
- If no recurrent Stridor after 2-3 hours from second neb, may discharge home
- Admit patient if recurrent Stridor after second Epinephrine neb
- Some admit if Stridor after first Epinephrine neb
- If no recurrent Stridor, may discharge home after 2-3 hours
- Indicated in moderate to severe emergency department cases with signs of respiratory distress
- Antibiotics
- Not indicated unless concurrent Bacterial Infection
- Helium added to Oxygen (Heliox)
- Not typically recommended
- Appears effective in small trials and my prevent intubation in borderline patients
- Requires mask delivery which may upset child and result in airway closure
- Consider with double set-up with Anesthesia to perform gas induction if sudden decompensation occurs
- Intubation
- See protocols below
- Indicated less frequently now with above management
- Significant risk of Subglottic Stenosis
- Use ET Tube at least 1 size smaller than predicted
XV. Management: Outpatient Management Indications
- Non-toxic appearance
- Well hydrated and taking oral fluids
- Minimal or no Stridor or retractions at rest
- At presentation or 3 hours after Epinephrine
- Reassuring respiratory Vital Signs
- Oxygen Saturation >94%
- Respiratory Rate <40 per minute
- Reliable parents
- Majority of croup patients may be discharged home
- However, keep a high index of suspicion for children with tenuous airways
- Croup can cause airway compromise that rivals Epiglottitis cases of the past
XVI. Management: Inpatient Observation Indications
- Persistent moderate to severe symptoms despite above management
- Dexamethasone 0.6 mg/kg and
- Epinephrine nebulizer treatment with observation for 3 hours (6 hours if a second Epinephrine given)
- Signs of respiratory distress or Respiratory Failure
- Cyanosis
- Tachypnea
- Agitation or Fatigue
- Stridor severity
- Accessory Muscle use
- Intercostal retractions
- Neck or abdominal Muscle use
- Rising arterial PCO2
XVII. Management: Severe Croup
- Risk of peri-respiratory arrest
- Notify Anesthesia (may require blow-by gas induction)
- Notify ENT or general surgery (may require emergent surgical airway)
- Notify PICU
- Avoid upsetting child
- May delay Dexamethasone until airway less tenuous (consider budesonide neb)
- Place in position of comfort sitting in parent's lap
- Non-invasive strategies
- Administer Racemic Epinephrine neb by blow-by
- Consider continuous Epinephrine neb in severe cases
- High Flow Nasal Cannula (HHFNC)
- Start at 2 L/kg/min and titrate as needed
- High Flow Oxygen via large bore nasal canula (with prewarmed air blended with compressed oxygen)
- Consider Ketamine for sedation (or intranasal Versed) to allow child to tolerate
- Consider Bipap
- Administer Racemic Epinephrine neb by blow-by
- Peri-respiratory arrest emergent airway management
- See Modified Delayed Sequence Intubation below
- Gas Induction or Ketamine IV if available
- Video Laryngoscopy (e.g. Glidescope)
- Load Elastic Bougie in mouth ready to pass through cords
- References
- Orman and Sloas in Majoewsky (2013) EM:Rap 13(2): 4-7
- Orman and Sloas in Herbert (2013) EM:Rap 15(6): 1-2
XVIII. Management: Modified Delayed Sequence Intubation
- Ketamine for sedation
- Continuous Epinephrine neb
- Pre-oxygenate (and expel carbon dioxide)
- High Flow Nasal Cannula (HHFNC) or
- BiPap mask attached to Ventilator set to SIMV with pressure support
- Set to RR 0-2 and TV 8-10 ml/kg
- Set Pressure support to 10-15 cmH2O and PEEP 5 cmH2O
-
Positive Pressure Ventilation
- Consider bilateral Nasal Airway trumpet (and if unconscious, Oral Airway)
- Consider Intubating Laryngeal Mask Airway (LMA)
- Provide Positive Pressure Ventilation via the LMA
-
Bag Valve Mask with PEEP Valve
- Use two provider technique (Luten Walls Technique)
- One provider squeezes bag with prolonged inspiratory phase and shorter expiratory phase
- Other provider achieves mask seal drawing Mandible up and holding mask tightly against face
- Intubate via pediatric bronchoscope
- Thread an under-sized Endotracheal Tube (ET) over pediatric bronchoscope
- Insert pediatric bronchoscope into the intubating LMA port
- Push ET Tube over the top of the bronchoscope through the Vocal Cords and remove the bronchoscope
- References
- Orman and Sloas in Majoewsky (2013) EM:Rap 13(2): 4-7
- Orman and Sloas in Herbert (2013) EM:Rap 15(6): 1-2
XIX. Management: Recurrent Croup
- Consider Esophageal Reflux
- Consider referral to pulmonology for bronchoscopy (especially age under 3 years old)
- Higher Incidence of findings such as Subglottic Stenosis or cyst
- Other risks include prior intubation, prematurity and age <3 years old
XX. References
- Cherry (2008) N Engl J Med 358(4): 384-91 [PubMed]
- Folland (1997) J Postgrad Med 101(3): 271-8 [PubMed]
- Geelhoed (1997) Pediatr Pulmonol 23:370-374 [PubMed]
- Klassen (1994) N Engl J Med, 331: 285-9 [PubMed]
- Knutson (2004) Am Fam Physician 69(3):535-42 [PubMed]
- Quan (1992) Am Fam Physician 46(3): 747-55 [PubMed]
- Sobol (2008) Otolaryngol Clin North Am 41(3): 551-66 [PubMed]
- Smith (2018) Am Fam Physician 97(9): 575-80 [PubMed]
- Wald (2010) Pediatr Ann 39(1): 15-21 [PubMed]
- Zoorab (2011) Am Fam Physician 83(9): 1067-73 [PubMed]
